Everything to Know About Shoulder Replacement Surgery
Introduction
Shoulder replacement surgery is a procedure designed to replace damaged or diseased shoulder joints with artificial ones. This surgery is typically recommended for individuals who are experiencing chronic shoulder pain or limited mobility due to conditions such as arthritis, fractures, or rotator cuff tears. By understanding the goal, types, preparations, procedure, recovery, complications, and outlook of shoulder replacement surgery, patients can make informed decisions about their health and well-being.
Goal
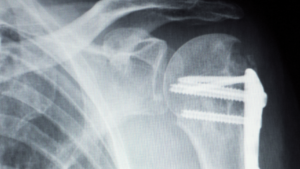
The primary goal of shoulder replacement surgery is to relieve pain and restore function to the shoulder joint. The procedure involves replacing the damaged joint surfaces with artificial components made of metal, plastic, or ceramic materials. By improving joint function and stability, shoulder replacement surgery aims to enhance the patient’s quality of life and enable them to regain their independence.
Who Needs It?
Shoulder replacement surgery is generally recommended for individuals who have severe shoulder pain or disability that has not responded well to conservative treatments such as physical therapy, medication, or other non-invasive interventions. People with degenerative joint diseases such as osteoarthritis or rheumatoid arthritis, as well as those with significant joint damage from injuries or fractures, might be candidates for shoulder replacement surgery. The decision to undergo this procedure is typically made in consultation with an orthopedic surgeon, who will assess the patient’s condition and determine if surgery is appropriate.
Types
There are several different types of shoulder replacement surgery, depending on the extent of the damage and the patient’s specific needs. The most common type is total shoulder replacement, where both the ball and socket portions of the joint are replaced. Another option is partial shoulder replacement, where only the ball or socket is replaced. In some cases, a reverse shoulder replacement may be advised for patients with significant rotator cuff tears or complex fractures. This procedure switches the positions of the ball and socket components, allowing other muscles to compensate for the damaged rotator cuff.
Preparations
Prior to shoulder replacement surgery, thorough preparations are essential to ensure a successful procedure and recovery. These preparations typically involve a comprehensive physical examination, blood tests, and imaging scans to assess the patient’s overall health and the extent of joint damage. It is important to inform the healthcare team about any medications, allergies, or pre-existing medical conditions to minimize the risk of complications. In some cases, the surgeon may recommend physical therapy or other interventions to improve muscle strength and flexibility before the surgery.
Procedure
During shoulder replacement surgery, the patient is placed under general anesthesia. The surgeon makes an incision to access the shoulder joint and removes the damaged bone and cartilage. The artificial components are then inserted and secured to the surrounding bone using specialized instruments and techniques. The incision is closed with stitches or staples, and a sterile bandage or dressing is applied. The duration of the surgery may vary depending on the complexity of the case, but it typically takes a few hours to complete.
Recovery
After shoulder replacement surgery, patients are closely monitored in the hospital for a few days. Physical therapy is an integral part of the recovery process, helping to restore range of motion, strength, and function in the shoulder. Pain medication and antibiotics may be prescribed to manage discomfort and prevent infections. It is important to follow the specific post-operative instructions provided by the surgeon. Rehabilitation typically continues for several weeks to months, gradually allowing the patient to resume activities and regain independence.
Complications
While shoulder replacement surgery is generally safe, there are potential complications associated with any surgical procedure. These can include infection, blood clots, nerve or blood vessel damage, temporary or permanent loss of shoulder function, and complications related to anesthesia. It is crucial to promptly report any unexpected symptoms or concerns to the healthcare team to ensure appropriate management and minimize the risk of complications.
Outlook
The outlook for individuals undergoing shoulder replacement surgery is generally positive. Many patients experience significant pain relief, improved range of motion, and better overall function in their shoulder joint. It is important to maintain a healthy lifestyle, follow a recommended exercise regimen, and attend regular follow-up appointments with the surgeon to monitor the long-term success of the surgery.
Summary
Shoulder replacement surgery is a procedure aimed at relieving pain and enhancing functionality for individuals with damaged shoulder joints. It is typically recommended for those who have not responded well to conservative treatments and are experiencing chronic pain or limited mobility. Various types of shoulder replacement surgery exist, including total shoulder replacement, partial shoulder replacement, or reverse shoulder replacement. Thorough preparations, including physical examinations and imaging scans, are necessary to ensure a successful surgery. Recovery involves close monitoring, physical therapy, and adherence to post-operative instructions. While complications may occur, the outlook for most patients is positive, with improved quality of life and reduced pain.